La apoplejía hipofisaria es una complicación poco frecuente de los adenomas de hipófisis, producida por un infarto hemorrágico o isquémico en el adenoma y con una clínica característica: cefalea intensa de comienzo agudo, alteraciones visuales y somnolencia o coma.
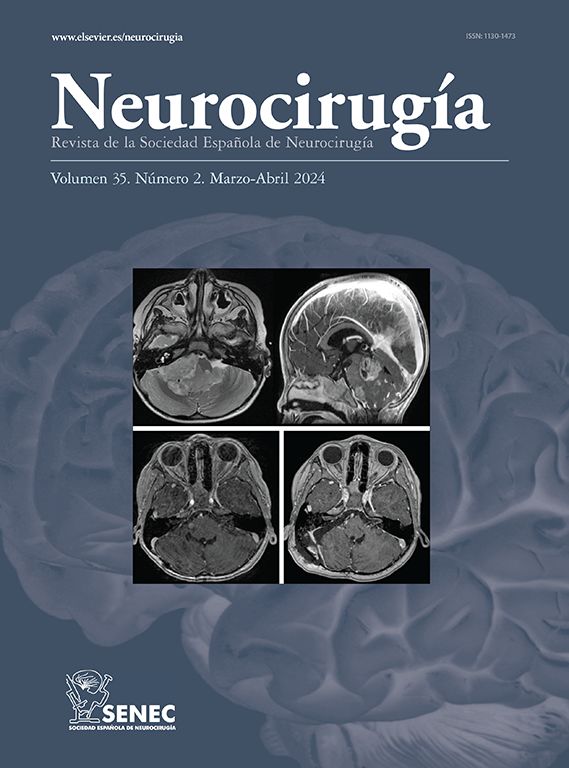
En los últimos 10 años hemos tratado a 8 pacientes con apoplejía hipofisaria. El diagnóstico fue clínico: 7 presentaron cefalea intensa y vómitos, 8 alteraciones visuales y 1 disminución del nivel de conciencia asociado a síndrome meníngeo. En 6 casos, la apoplejía fue la primera manifestación del adenoma de hipófisis. La resonancia magnética y la tomografía computada demostraron el ictus hipofisario en 7 pacientes. La cirugía descompresiva transesfenoidal se efectuó en 7 casos, sólo en uno de urgencia. Todos presentaron una significativa recuperación de las alteraciones visuales, sin embargo, en ninguno se observó mejoría de las alteraciones endocrinológicas preoperatorias.
Consideramos que el diagnóstico precoz, el rápido inicio del tratamiento hormonal sustitutivo y la cirugía transesfenoidal urgente o diferida en función de la clínica, deben ser la base del tratamiento adecuado de la apoplejía hipofisaria.
Pituitary apoplexy is an infrequent complication of pituitary adenomas, caused by hemorrhagic or ischemic infarction in the tumor, with typical clinical presentation: severe headache of sudden onset, visual disturbances, sleep tendency or comma.
Along the last ten years we have treated eight patients with pituitary apoplexy. The diagnostic was clinically established in all of them. Seven cases com-plained of severe headache and vomiting. Eight patients reported visual disturbances. In one case low level of consciousness and meningeal irritation were the only findings. In six cases the apoplexy was the first pituitary adenoma manifestation. MRI and CT studies demons-trated the pituitary stroke in seven patients.
Surgical trans-sphenoidal decompression was performed in seven patients, requiring urgent management in only one case.
All patients experienced a marked visual improvement, but there was no amelioration of endocrine preoperative disturbances in any case. We conclude that quick diagnosis, early onset of hormonal therapy and urgent or delayed trans-sphenoidal surgery, depending on clinical manifestations, constitute the principies of the appropriate treatment of pituitary apoplexy.
Artículo

Si es la primera vez que accede a la web puede obtener sus claves de acceso poniéndose en contacto con Elsevier España en suscripciones@elsevier.com o a través de su teléfono de Atención al Cliente 902 88 87 40 si llama desde territorio español o del +34 932 418 800 (de 9 a 18h., GMT + 1) si lo hace desde el extranjero.
Si ya tiene sus datos de acceso, clique aquí.
Si olvidó su clave de acceso puede recuperarla clicando aquí y seleccionando la opción "He olvidado mi contraseña".
Comprando el artículo el PDF del mismo podrá ser descargado
Precio 19,34 €
Comprar ahora