Craniopharyngiomas are a big challenge in the neurosurgical field. Because these lesions involve important systems, surgeons must weigh the risks of aggressive resection against the long-term challenges of recurrence. We present the outcomes of our patients based on clinical results, degree of resection, recurrence and disease-free survival.
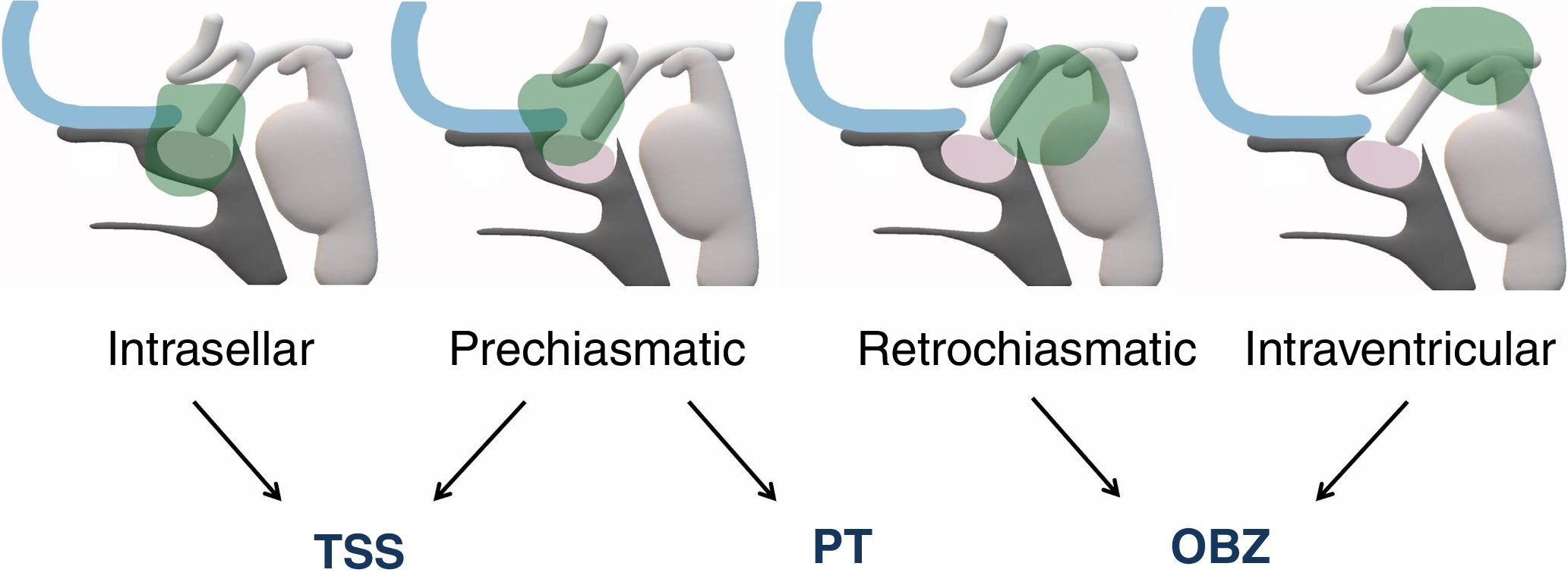
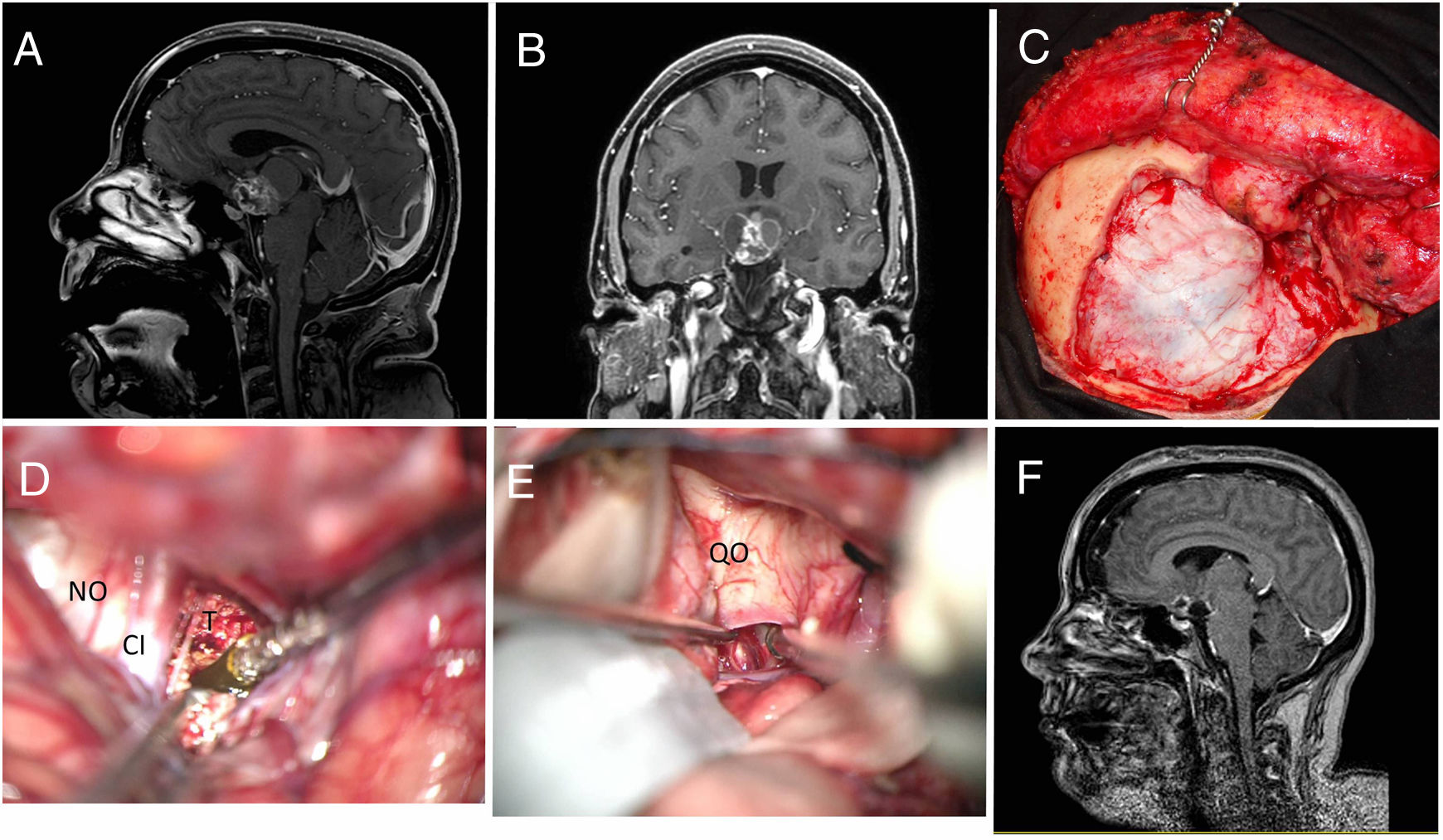
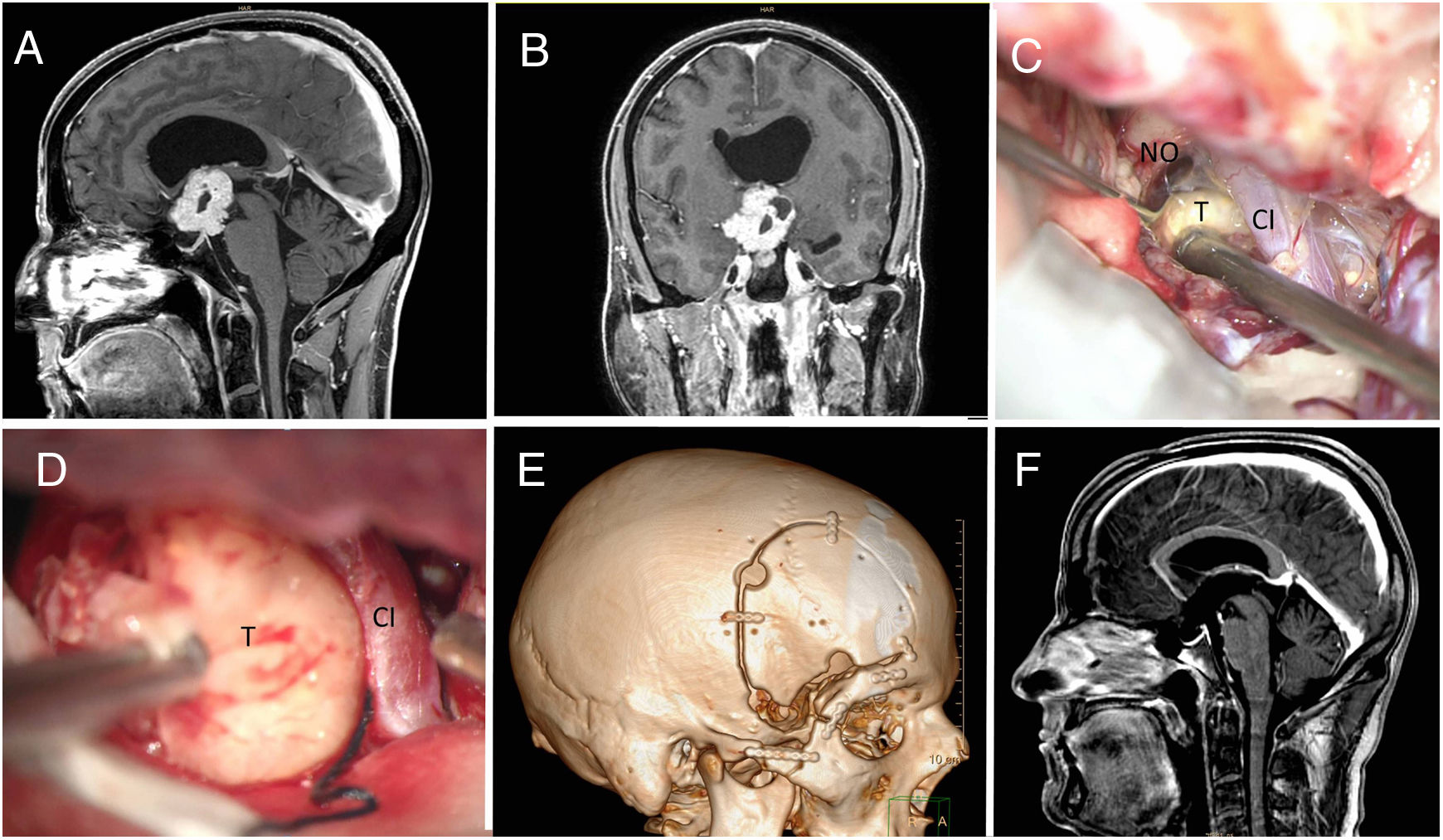
Materials and methodsWe reviewed medical records in all patients who had undergone surgical resection for craniopharyngioma at (Institution’s name) between 2007 and 2019. We considered ophthalmological examinations, imaging studies, endocrinological studies and surgical complications. Radical resections were planned in all of the patients. To help choose the correct surgical approach, craniopharyngiomas were classified based on tumour location.
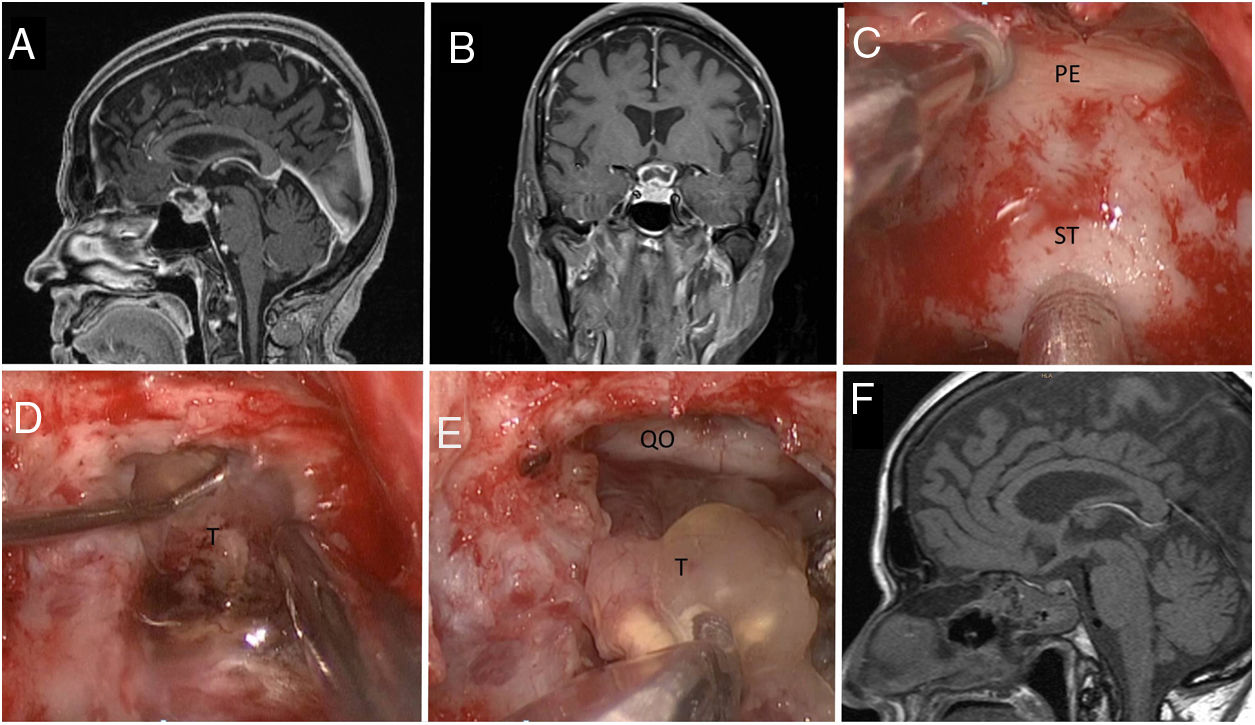
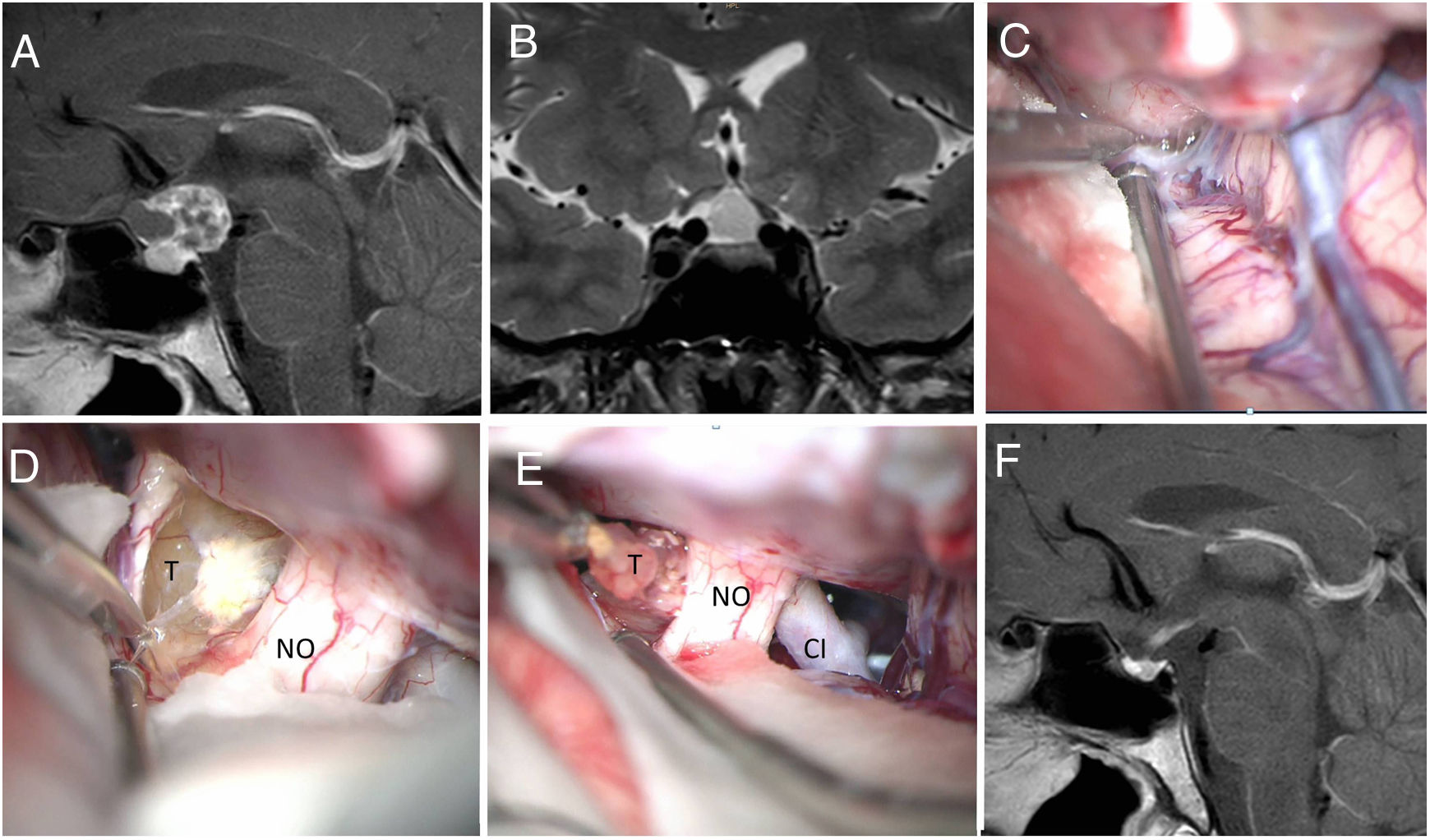
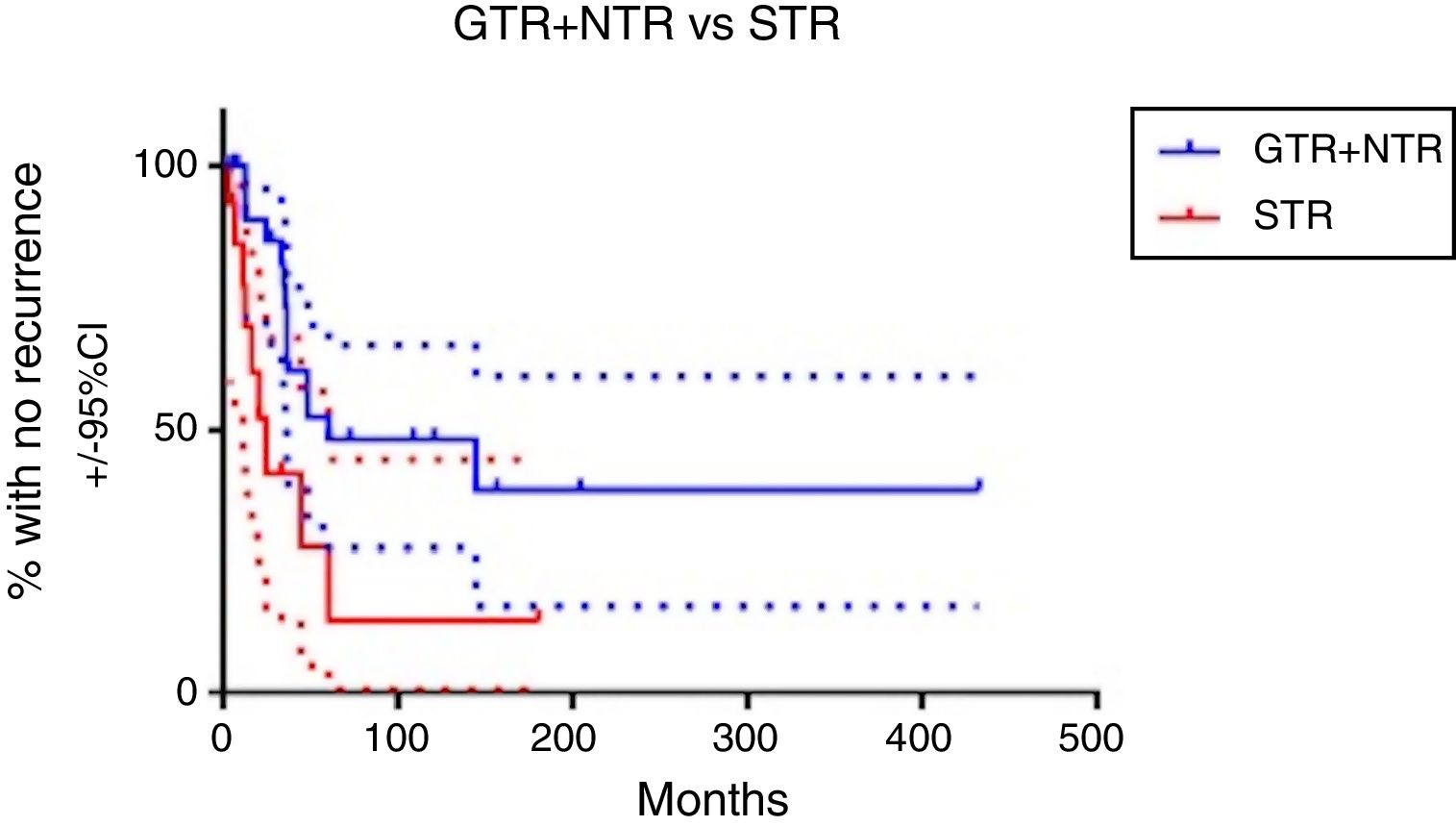
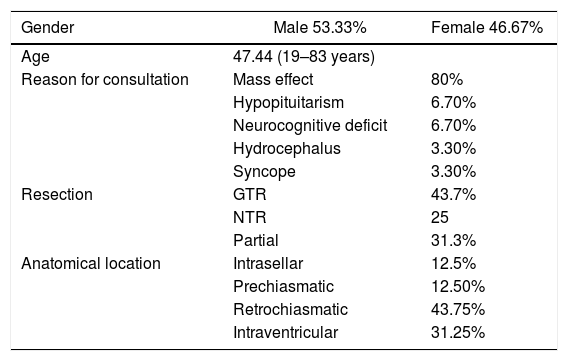
ResultsThirty cases of craniopharyngioma were analysed. 12.5% were classified as intrasellar, 12.5% as prechiasmatic, 43.75% as retrochiasmatic, and 31.25% as intraventricular. Overall, 38 cases involved a transcranial surgery (15 orbitozygomatic approach; 19 pterional approach and 4 transcallosal approach), 7 involved a transsphenoidal approach, 2 microscopic transnasal approach and one ventricular endoscopy for emptying the craniopharyngioma cyst. Gross-total resection was achieved in 43.7% and near-total resection (more than 90%) in 25%. The mean follow-up period after resection was 4.7 years. Tumour recurrence occurred in 48%, with an average of 42.7 disease-free months.
ConclusionTotal tumour resection is the best treatment for craniopharyngioma. Due to its high morbidity and mortality, a multidisciplinary team is necessary for the management of these tumours.
Los craneofaringiomas son un gran desafío en el campo neuroquirúrgico. Debido a que estas lesiones involucran estructuras importantes, los cirujanos deben sopesar los riesgos de una resección agresiva frente a los desafíos de la recurrencia a largo plazo. Presentamos los resultados de nuestra serie de pacientes en función de los resultados clínicos, el grado de resección, la recurrencia y la supervivencia libre de enfermedad.
Materiales y métodosse revisaron las historias clínicas de todos los pacientes que se sometieron a una resección quirúrgica por craneofaringioma en el (nombre de la institución) entre 2007 y 2019. Se consideraron los exámenes oftalmológicos, estudios de imágenes, estudios endocrinológicos y complicaciones quirúrgicas. En todos los pacientes se planificaron resecciones totales. Para la correcta elección del abordaje quirúrgico, los craneofaringiomas se clasificaron según su ubicación.
ResultadosSe analizaron treinta pacientes con diagnóstico de craneofaringioma. El 12,5% se clasificó como intraselar, el 12,5% como prequiasmático, el 43,75% como retroquiasmático y el 31,25% como intraventricular. En total, 38 casos incluyeron una cirugía transcraneal (15 abordaje orbitocigomático; 19 abordaje pterional y 4 abordaje transcalloso), 7 incluyeron abordaje transeptoesfenoidal, 2 abordajes transnasales microscópicos y una endoscopia ventricular para vaciar el quiste craneofaringioma. La resección total se logró en el 43,7% de los pacientes y la resección casi total (mayor al 90%) en el 25%. El período de seguimiento promedio después de la resección fue de 4,7 años. La recurrencia tumoral ocurrió en el 48%, con un promedio de meses libres de enfermedad de 42,7.
ConclusiónLa resección tumoral total es el mejor tratamiento para los craneofaringiomas. Debido a su alta morbilidad y mortalidad, se necesita un equipo multidisciplinario para el manejo de estos tumores.
Article

If it is the first time you have accessed you can obtain your credentials by contacting Elsevier Spain in suscripciones@elsevier.com or by calling our Customer Service at902 88 87 40 if you are calling from Spain or at +34 932 418 800 (from 9 to 18h., GMT + 1) if you are calling outside of Spain.
If you already have your login data, please click here .
If you have forgotten your password you can you can recover it by clicking here and selecting the option ¿I have forgotten my password¿.